Press release

NOBELFÖRSAMLINGEN KAROLINSKA INSTITUTET
THE NOBEL ASSEMBLY AT THE KAROLINSKA INSTITUTE
The Nobel Assembly at the Karolinska Institute has today decided to award the Nobel Prize in Physiology or Medicine for 1985 jointly to
Michael S. Brown and Joseph L. Goldstein
for their discoveries concerning “the regulation of cholesterol metabolism”.
Summary
Michael S. Brown and Joseph L. Goldstein have through their discoveries revolutionized our knowledge about the regulation of cholesterol metabolism and the treatment of diseases caused by abnormally elevated cholesterol levels in the blood. They found that cells on their surfaces have receptors which mediate the uptake of the cholesterol-containing particles called low-density lipoprotein (LDL) that circulate in the blood stream. Brown and Goldstein have discovered that the underlying mechanism to the severe hereditary familial hypercholesterolemia is a complete, or partial, lack of functional LDL-receptors. In normal individuals the uptake of dietary cholesterol inhibits the cells own synthesis of cholesterol. As a consequence the number of LDL-receptors on the cell surface is reduced. This leads to increased levels of cholesterol in the blood which subsequently may accumulate in the wall of arteries causing atherosclerosis and eventually a heart attack or a stroke.
Brown and Goldstein’s discoveries have lead to new principles for treatment, and prevention, of atherosclerosis.
Cholesterol – an important substance
The cholesterol debate during the last decade may have given the public the impression that cholesterol is something you have to avoid to survive. This is, however, neither possible nor desirable: cholesterol is present in all our tissues and is produced in the body. Cholesterol is also vitally important for several of the normal processes in the body.
Cholesterol originates from two main sources – from within through biosynthesis predominantly in the liver, and from without through fat in the food. In the liver as well as in the intestine cholesterol is packeted into particles in such a way that it can be transported in the blood and lymphatic fluid. These particles are called lipoprotein – a combination of fat and proteins. There are different kinds of lipoproteins and they are classified on the basis of their density as determined by ultracentrifugation: Low Density Lipoproteins (LDL), Very Low Density Lipoproteins (VLDL) and High Density Lipoproteins (HDL). The particles transporting cholesterol circulating in the blood are LDL.
LDL, the major cholesterol carrier in the blood, is a spherical particle (Figure 1). Its core consists of some 1,500 cholesteryl esters, each a cholesterol molecule attached by an ester linkage to a long fatty acid chain. The oily core is shielded from the aqueous plasma by a coat composed of unesterified cholesterol, phospholipid and one large protein molecule, apoprotein B. The apoprotein B molecule moors the LDL to specific receptors on the cell surface – the LDL-receptor.
A normal healthy person has approximately 2 g cholesterol per liter plasma. The highest abnormal values, approximately 10 g per liter, are found in persons with a severe disease called familial hypercholesterolemia (FH), which is an inborn error of metabolism.
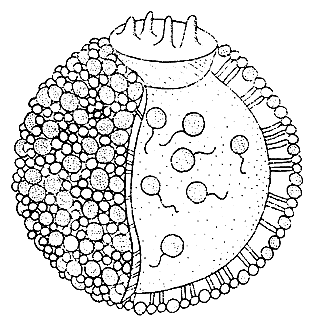 |
Figure 1. The LDL is a spherical particle with a radius of one millionth millimeter. Most of the cholesterol in the blood stream is found in LDL particles. Its core consists of approximately 1,500 cholesteryl esters, each a cholesterol molecule attached by an ester linkage to a long fatty acid chain. The core is surrounded by a surface coat composed of 800 molecules of phospholipid, 500 molecules of unesterified cholesterol and one large protein molecule, apoprotein B, which moors the LDL to the receptor on the cell surface.
Cholesterol is found in cell membranes and is converted to hormones and bile acids
Cholesterol has two main functions in the body. It constitutes a structural component in cell membranes, and it is converted to certain steroid hormones and bile salts. More than 90 per cent of the cholesterol in the body is found in cell membranes.
Each cell is surrounded by a membrane, the cell or plasma membrane. Its function is not only to be a protective coat. It also serves as a border control determining which substances are allowed to enter or leave the cell. This function is sometimes facilitated by the presence of specific receptors whereby certain molecules are efficiently trapped and taken up by the cell.
The cells either produce their own cholesterol or take up LDL circulating in the blood stream. The discovery of the LDL-receptor by Brown and Goldstein in 1973 was a milestone in cholesterol research.
Several hormones are produced from cholesterol like estrogen and testosteron, cortison and aldactone. Cholesterol is stored in cells of the adrenals and gonads and can be utilized as soon as there is a requirement for these hormones.
Cholesterol also takes part in the synthesis of vitamin D which prevents development of rickets. Vitamin D is produced in the skin when exposed to the sun’s ultraviolet light.
Another vital function of cholesterol is associated with food intake. Cholesterol is converted into bile acids in the liver and is transported via the bile to the upper intestine where the bile salts emulsify the dietary fat making it absorbable. The bile salts then return to the blood stream and are taken up by the liver and again secreted into the upper intestine. This recycling of bile acids normally limits the liver’s need for cholesterol.
Excess cholesterol accumulates in the walls of arteries
As stated above cholesterol is of vital importance for the body. Thus, cholesterol deficiency, a rare disease, causes severe damage particularly in the nervous system. However, the most common abnormality in the cholesterol metabolism is of the opposite kind. Excess cholesterol accumulates in the walls of arteries forming bulky plaques that inhibit the blood flow until a clot eventually forms, obstructing the artery and causing a heart attack or stroke.
The accumulation of cholesterol in the arterial walls is a slow process lasting over decades. Among factors contributing and accelerating this process are high blood pressure, a high intake of animal fat in the food, smoking, stress and genetic factors.
Studies on patients with familial hypercholesterolemia (FH) by Michael S. Brown and Joseph L. Goldstein constitute founding stones for our present knowledge concerning the cholesterol metabolism. FH exists in different forms and is inherited as a monogenic dominant trait. Individuals who carry the mutant gene in double dose (homozygotes) are severely affected. Their serum cholesterol levels are five times higher than in healthy persons, and severe atherosclerosis and coronary infarction is seen already in adolescence, or even earlier. Individuals who have inherited only one mutant gene (heterozygotes) develop symptoms later in life – at 35 to 55 years of age. Their cholesterol levels are approximately 2-3 times higher than in normal people.
Patients with FH lack functional LDL-receptors
Brown and Goldstein studied cultured human cells (fibroblasts) from healthy individuals and individuals with FH. Like all animal cells cultured fibroblasts need cholesterol in their cell membranes. Cholesterol – in the form of LDL – was found to be taken up by highly specific receptor molecules on the cell surface – the LDL-receptor. The revolutionizing discovery was then made that fibroblasts from patients with the most severe form of FH completely lacked functional LDL-receptors. Fibroblasts from patients with the milder form of FH had fewer LDL-receptors than normal – a reduction by half.
Brown and Goldstein also discovered that the synthesis of cholesterol in normal fibroblasts was inhibited when LDL-containing serum was added to the cell culture. Fibroblasts from homozygous patients with FH were not inhibited since they lacked functional LDL-receptors. Consequently their intracellular synthesis could not be influenced.
In later studies Brown and Goldstein showed that LDL which had bound to the receptor was taken up by the cells as a LDL-receptor complex. The receptor is localized on the cell surface in what is called a coated pit. The coated pit invaginates and pinches off to form a coated vesicle (Figure 2). Fusion of several vesicles gives rise to an endosome. The entire process is named receptor-mediated endocytosis. The cholesterol in the LDL particle is released inside the cell. One effect of the uptake of cholesterol is that it inhibits the manufacture of new LDL-receptors on the cell surface. A reduced number of LDL-receptors leads to a diminished LDL uptake. LDL then remains in the blood stream with the risk of accumulation in the arterial walls.
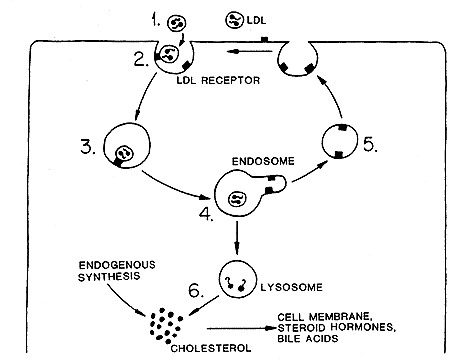
Figure 2. The cells uptake of LDL particles circulating in the blood (1) starts with their mooring to LDL-receptors in coated pits (2) on the cell surface. These pits invaginate and pinch off to form coated vesicles (3). Fusion of vesicles gives rise to an endosome (4) in which the LDL dissociates from the receptor, which is recycled (5) to the surface. The LDL is delivered to a lysosome where the cholesteryl ester is cleaved to yield free cholesterol to be utilized for membrane synthesis or is converted to steroid hormones and bile acids. Cholesterol taken up by the cell inhibits the cell’s own cholesterol synthesis.
Brown and Goldstein have discovered a new, and unexpected way of regulation of cholesterol metabolism. Normally cells have a high capacity to synthesize their own cholesterol. With a low availability of cholesterol (LDL) in the blood circulation the cells increase the number of LDL-receptors on their surface. The concentration of LDL in the blood is thereby diminished. The more LDL there is in the blood circulation the easier it is for the cells to acquire it. With a high dietary fat intake an excess of LDL circulates in the blood.
The discoveries have resulted in new approaches for the treatment of atherosclerosis
The discovery of the LDL-receptor has broadened our understanding of cholesterol metabolism considerably and explained the mechanism behind familial hypercholesterolemia.
Brown and Goldstein have used modern molecular biology techniques to show that the LDL-receptor is a glycoprotein located in the cell membrane. Its protein part is constructed by 839 amino acids. Of these 767 are localized on the cell surface, 22 within the membrane and 50 inside the cell in the cytoplasma (Figure 3). The LDL-receptor defect can be one of several different kinds: in some cases the receptor is completely lacking, in others LDL binds poorly, or not at all, to receptor and in still others LDL is bound to the receptor but the LDL-receptor complex is not internalized. Analysis of the LDL-receptor in two patients have shown changes in the intracellularly located protein part of the glycoprotein: in one patient out of the expected number of 50 amino acids only two were present, in another 6 “correct” but 8 “wrong” amino acids were present. The part of the receptor located on the cell surface was unaltered in both patients.
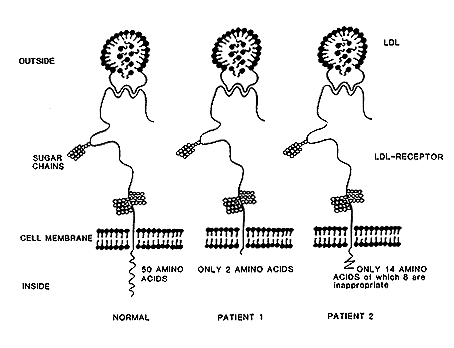 |
Figure 3. LDL-receptors, one healthy and two abnormal. The part of the receptor localized outside the cell membrane is identical in all three cases. The difference is found in the portion of the receptor inside the cell membrane. The healthy receptor is to the left in the figure. When the LDL via its apoprotein moors to the receptor it is internalized by the normal healthy receptor. The two abnormal receptors are unable to complete the internalization.
The severe form of FH (homozygous) is rare, about one in a million people. The milder form of FH (heterozygous) is much more common, about one in 200-500 people. This means that in a city like Stockholm several thousand inhabitants have the disease with its associated risks of atherosclerosis and heart infarction.
Brown and Goldstein have introduced entirely new principles for treatment of FH based on their discovery of the LDL-receptor. In individuals with the milder heterozygous form of FH the number of LDL-receptors has been increased using drugs – cholestyramine and mevinolin. Such treatment has been found to lower blood cholesterol levels. In the more severe homozygous form of FH, where functional LDL-receptors are missing, medication is no therapeutic alternative. There liver transplantation has been tried. A severely ill 6 year old girl, who already had suffered several heart attacks, was given a new liver and heart simultaneously. More than six months after the operation her blood cholesterol levels were in the range of 3 g per liter compared to 12 g per liter before the liver transplantation.
The discoveries made by Brown and Goldstein have drastically widened our understanding of the cholesterol metabolism and increased our possibilities to prevent and treat atherosclerosis and heart attacks. But their discoveries have even more far-reaching implications. Coronary infarction is a major cause of death in most industrialized countries. The disease is caused by hereditary and environmental factors, which together cause a reduction of the number of LDL-receptors. This increases the blood levels of LDL and thereby the risk for atherosclerosis. Brown and Goldstein’s revolutionary results have widened our horizon and holds promise for future fascinating developments. They speculate themselves about therapy with drugs that increase the number of LDL-receptors simultaneous with a lesser demand for dietary regimens … “it may one day be possible for many people to have their steak and live to enjoy it too”.
References
L. A. Carlson: Det goda och det onda serumkolesterolet. Nya synpunkter på de olika lipoproteinkolesterolernas betydelse för åderförkalkningssjukdomarna. Medicinsk Årbog, Munksgaard, Köpenhamn, 1980, pp. 201-209.
M. S. Brown, J. L .Goldstein: How LDL Receptors Influence Cholesterol and Atherosclerosis. Scientific American 1984, 251, pp. 52-60.
Nobel Prizes and laureates
Six prizes were awarded for achievements that have conferred the greatest benefit to humankind. The 14 laureates' work and discoveries range from quantum tunnelling to promoting democratic rights.
See them all presented here.
