Emil von Behring
Article

Emil von Behring: The founder of serum therapy
Based on an exhibition at Marburg Castle
arranged and documented by Kornelia Grundmann*
This article was published on 3 December 2001.
Upbringing and education
Emil Behring (1854-1917) was born on March 15, 1854 in Hansdorf, West Prussia, as the first child of the couple August and Auguste Behring. His father was a village school teacher, who during his first marriage had had four children and after the birth of Emil had another eight children.
A talented pupil, Emil Behring was above all assisted by the village minister, who made it possible for him to attend the Gymnasium (High School) in the village Hohenstein. His orientation as a theology student appeared to have changed after a friend who was a military doctor arranged for him to start his medical studies at the University of Berlin. He obtained a scholarship and from 1874 through 1878 he studied at the Academy for Military Doctors at the Royal Medical-Surgical Friedrich-Wilhelm-Institute, where he also earned his medical degree. In the following years he had to perform as a military doctor and also worked as a troop doctor in various garrisons. After having been assigned as captain of the medical corps to the Pharmacological Institute at the University of Bonn, he was given a position at the Hygiene Institute of Berlin in 1888 as an assistant to Robert Koch (1843-1910), one of the pioneers of bacteriology. During this time, Behring’s first authoritative publication on diphtheria and tetanus serum therapy appeared.

Emil von Behring in a military uniform.
The Behring family
During his early years as a military doctor, Behring’s income was not sufficient for him to think about starting a family. Only in 1896, when he had a regular salary, did he marry the 20 year old Else Spinola. They went on a three-month honeymoon to the island of Capri. Else, born August 30, 1876 in Berlin, was the daughter of Werner Spinola, Administrative Director of Charité, the university medical clinic in Berlin.
In 1898, after having become professor at the University in Marburg (then part of Prussia), Behring moved with his family into a house in Wilhelm-Roser-Strasse in Marburg, where his six sons were born. Behring was a family man, though rather patriarchal, which at that time was quite normal. In the circle of his family he felt content, although his scientific work presumably did not leave him much time for his wife and children.

Wedding picture of Emil and Else von Behring.
On March 31, 1917, Behring died and was entombed in a mausoleum at the Marburg Elsenhöhe. After Behring’s death, Else von Behring served as chairwoman of the Women’s National Organisation in Marburg, Germany. She died in 1936 of a heart attack at the age of only 59.
Family and friends
On the list of his sons’ godfathers, it appears obvious who stood closest to Emil von Behring besides his family. His first son, Fritz, had the bacteriologist Friedrich Loeffler (1852-1915) and Behring’s friend and co-worker, Erich Wernicke as godfathers. The godfather of his third son, Hans, was the Prussian Under-Secretary of Education and Cultural Affairs, Friedrich Althoff. His fifth son, Emil, had as a godfather the Russian researcher Elias Metschnikoff (1845-1916), founder of the theory of phagocytosis, with whom Behring had continuous scientific exchange of ideas. Emil’s second godfather was the pupil of Louis Pasteur, Émile Roux (1853-1933), who like Behring Sr. dealt with the fight against diphtheria. In 1913, the godfather of his sixth son, Otto, was the physician Ludolph Brauer (1865-1951), who had taught together with Behring at the Marburg Medical Faculty as a professor of internal medicine.
The development of the diphtheria-therapeutic-serum
Behring, who in the early 1890s became an assistant at the Institute for Infectious Diseases, headed by Robert Koch, started his studies with experiments on the development of a therapeutic serum. In 1890, together with his university friend Erich Wernicke, he had managed to develop the first effective therapeutic serum against diphtheria. At the same time, together with Shibasaburo Kitasato he developed an effective therapeutic serum against tetanus.

Behring together with his colleagues Wernicke (left) and Frosch (center) in Robert Koch’s laboratory in Berlin.
The researchers immunized rats, guinea pigs and rabbits with attenuated forms of the infectious agents causing diphtheria and alternatively, tetanus. The sera produced by these animals were injected into non-immunized animals that were previously infected with the fully virulent bacteria. The ill animals could be cured through the administration of the serum. With the blood serum therapy, Behring and Kitasato firstly used the passive immunization method in the fight against infectious diseases. The particularly poisonous substances from bacteria – or toxins – could be rendered harmless by the serum of animals immunized with attenuated forms of the infectious agent through antidotes or antitoxins.

Shibasaburo Kitasato.
The introduction of serum therapy
The first successful therapeutic serum treatment of a child suffering from diphtheria occurred in 1891. Until then more than 50,000 children in Germany died yearly of diphtheria. During the first few years, there was no successful breakthrough for this form of therapy, as the antitoxins were not sufficiently concentrated. Not until the development of enrichment by the bacteriologist Paul Ehrlich (1854-1915) along with a precise quantification and standardization protocol, was an exact determination of quality of the antitoxins presented and successfully developed. Behring subsequently decided to draw up a contract with Ehrlich as the foundation of their future collaboration. They organized a laboratory under a railroad circle (Stadtbahnbogen) in Berlin, where they could then obtain the serum in large amounts by using large animals – first sheep and later horses.
In 1892, Behring and the Hoechst chemical and pharmaceutical company at Frankfurt/Main, started working together, as they recognized the therapeutic potential of the diphtheria antitoxin. From 1894, the production and marketing of the therapeutic serum began at Hoechst. Besides many positive reactions, there was also noticeable criticism. Resistance, however, was soon put aside, due to the success of the therapy.
The Marburg years
Behring was given the opportunity to start a university career through one of the leading officers (Ministerialrat) of the Prussian Ministry of Education and Cultural Affairs, Friedrich Althoff (1839-1908), who wanted to improve the control of epidemics in Prussia by supporting bacteriological research. After a short period as professor at the University of Halle-Wittenberg, Behring was recruited by Althoff to take over the vacant chair in hygiene at Philipps Marburg University on April 1, 1895. His appointment as full professor followed shortly thereafter against the will of the faculty, who besides all of Behring’s outstanding discoveries, wanted a university lecturer who would broadly represent the field. However, Althoff rejected all counterproposals and Behring took over as Director of the Institute of Hygiene at Marburg. His position included giving lectures for hygiene and concurrently held a teaching contract in the history of medicine. In 1896, the Marburg Institute of Hygiene moved to a building on a road nearby Pilgrimstein Road, previously the Surgery Clinic. Behring divided the Institute into two departments, a Research Department for Experimental Therapy and a Teaching Department for Hygiene and Bacteriology. He remained Director of the Institute until his retirement as professor in May 1916.
Scientific contacts
Behring belonged to a scientific discussion group called “The Marburg Circle” (das Marburger Kränzchen), whose other members were the zoologist Eugen Korschelt (1858-1946), the surgeon Paul Friedrich (1864-1916), the botanist Arthur Meyer (1850-1922), the physiologist Friedrich Schenk (1862-1916), the pathologist Carl August Beneke (1861-1945) and the pharmacologist August Gürber (1864-1937). They often met at Behring’s home where they had rounds of vivid and prolific scientific discussions.
Active protective vaccination against diphtheria
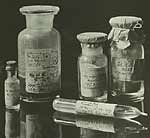
Old vials (1897 and 1906) with hand-written labels.
The therapeutic serum developed by Behring prevented diphtheria for only a short period of time. In 1901, Behring, therefore, for the first time, used a diphtheria innoculation of bacteria with reduced virulence. With this active immunization he hoped to help the body also produce antitoxins. As a supporter of the humoral theory of immune response, Behring believed in the long-term protective action of these antitoxins found in serum. It is well-established knowledge today that active vaccination stimulates the antitoxin (antibody) producing cells to full function.
The development of an active vaccine took a few years. In 1913, Behring went public with his diphtheria protective agent, T.A. (Toxin-Antitoxin). It contained a mixture of diphtheria toxin and therapeutic serum antitoxin. The toxin was meant to cause a light general response of the body, but not to harm the person who is vaccinated. In addition, it was designed to provide long-term protection. The new drug was tested at various clinics and was proven to be non-harmful and effective.
Tetanus therapeutic serum during World War I
In 1891, tetanus serum was introduced considerably more quickly in clinical practices than the diphtheria serum. The Agricultural Ministry supported research efforts to develop a therapeutic agent against tetanus to protect agriculturally valuable animals. The large amounts of serum required were obtained through the immunization of horses. However, there was no substantial clinical testing on humans; this led the Military Administration to accept it only on a small scale at the beginning of World War I.
During the first months of the war, this restraint led to massive losses of human lives. Also, after the distribution of the tetanus antitoxins in the military hospitals, many futile attempts at therapy were noted. At the end of 1914, as a result of Behring’s constructive assistance, the injection of serum was established as preventing disease. Starting in April 1915, the mistakes in dosage and the shortage of supplies were overcome and the numbers of sick fell dramatically. Behring was declared “Saviour of the German Soldiers” and was awarded the the Prussian Iron Cross medal.

Historical engraving showing how the medicinal serum was obtained from immunized horses.
An attempt to develop a therapeutic method against tuberculosis
After Robert Koch had failed with his tuberculosis therapy in 1893, Behring began to search for an effective therapeutic agent against this disease. However, very soon, he had to admit that combating tuberculosis using a healing serum was not feasible. Therefore, he concentrated on working on a preventive vaccination, which, however, required precise knowledge of the mechanism of infection. In Behring’s view, the tubercle bacillus was transmitted to children through the milk of a mother or a cow infected with tuberculosis. He then started treating milk with formaldehyde, so as to eliminate this source of infection. This procedure was not accepted due to the bad smell of the milk. Moreover, the transmission of tubercle bacilli through the respiratory tract was proven to be more likely than through the digestive system, as had been claimed by Behring.
From 1903, Behring worked on active immunization through attenuated tuberculosis infectious agents, which he then tried on cows, however, with only moderate success. His aim was to obtain a protective and therapeutic agent for humans. A number of agents (tuberculase, tulase, tulaseactin, tulon) failed to make a breakthrough. At the beginning of World War I, Behring halted his efforts to combat tuberculosis and dedicated himself entirely to the further development of tetanus serum.
Behring’s relationship to Paul Ehrlich
Paul Ehrlich was Behring’s colleague at Robert Koch’s institute. Here, he was able to work out a reliable and reproducible standardization method for diphtheria serum. However, in later years, tension developed between the two researchers. Differences with Ehrlich’s pupil, Hans Aronson, resulted in bad feelings, which increased when Ehrlich’s Royal Institute of Experimental Therapy was founded at Frankfurt/Main. The previous friendship between the two researchers never fully succumbed, through the mediation of Friedrich Althoff. However, it was subsequently demonstrated that the only photograph showing Behring and Ehrlich together, which appeared on the cover of a Berlin newspaper on the occasion of their 60th birthday in 1914, was a photomontage made up of two separate photographs.

Report of the Berliner Illustrirte Zeitung (Berlin Illustrated Newspaper) about Emil von Behring and Paul Erlich and their work on the occasion of their 60th birthday.
Behring’s health
Behring lived entirely for his idea of revolutionizing medicine through serum therapy. This idea hung above him and motivated him, in his own words, “like a demon.” His enormous concentration on his work often drove him to physical illnesses, as well as to deep depressions, which forced him to take time off work for a sanatorium stay from 1907 through 1910.
Acknowledgements and honors
In 1903, Emil von Behring was given the title of “Wirklicher Geheimer Rat mit dem Prädikat Excellenz” by the German emperor Wilhelm II. The diploma says: “This is in order that Behring should remain in unbroken loyalty to Myself and the Royal Family and to fulfill his official responsibility with continuous eagerness, whereby he who has the right connected to his present character, will receive the highest protection by Myself”. A splendid uniform was provided along with the title.
In 1901, when the Nobel Prizes were awarded for the first time, Behring received the Prize in Physiology or Medicine.

A detail (right) and the diploma for the first Nobel Prize in Physiology or Medicine, awarded to Behring in 1901.
Behring jubilee in 1940
On December 4, 1940, the Philipps University Marburg celebrated the 50th anniversary of the original publication of Emil von Behring’s decisive discovery of serum therapy. Top leaders of the National Socialist Party, the rectors of numerous German universities, representatives of the Behringwerke and many scientists and friends of Emil von Behring from abroad were also present. The celebration, which continued over a few days, began with lectures and addresses by officials, both of the state and party. Finally, a foundation certificate for a new Institute for Experimental Therapy was handed over. The professors then moved from the university auditorium (Aula), to unveal a new Behring Memorial close to the St. Elisabeth Church. The celebration was followed by a two-day scientific meeting, presenting the state of the art of immunology and the fight against infectious diseases.
The background of the celebration
In the view of the National Socialists, Else von Behring was regarded as a “half-Jew”, as her mother came from a Jewish family. With the help of a number of friends she was able to get her sons accepted by Hitler as “Aryans” and not stigmatized as “half-breeds”. After the death of Else von Behring in 1936, no obstacles were left for the Nazi party to use Emil von Behring as a glorified representative of national socialist “Germanic” science. During the ceremony there were, however, some signs of tension. Although one of Behring’s sons participated in the ceremony, he was not greeted by any of the official speakers. Only the Danish researcher, Thorvald Madsen from Copenhagen, who had previously been chairman of the Health Organisation of the League of Nations, dared to mention Behring’s friendly connection with researchers from enemy countries, such as those at the Institut Pasteur in Paris. Courageously, he also recalled the great bacteriologist Paul Ehrlich, despised by the Nazis due to his Jewish origin, who had played a significant role in Behring’s successes.
Translated by Gabriella Nichols, Department of Anatomy, Philipps University Marburg, Germany.
* The exhibition was from October to December 2001.
Kornelia Grundmann (b. 1951) studied biology, biochemistry and medicine at the Free University of Berlin and worked for close to ten years in biomedical research. Subsequently she moved to Marburg and began research in the history of medicine focusing on the 19th and 20th century (anatomy, bacteriology and psychiatry). In particular, she has studied the development of the medical faculty of Marburg during the Third Reich and the postwar period.
Dr Grundmann is curator of the Behring Archives at the Behring Library for History and Ethics of Medicine and the Anatomical Museum of the Phillips University, Marburg, Germany.
First published 3 December 2001
Nobel Prizes and laureates
Six prizes were awarded for achievements that have conferred the greatest benefit to humankind. The 14 laureates' work and discoveries range from quantum tunnelling to promoting democratic rights.
See them all presented here.
