Press release

NOBELFÖRSAMLINGEN KAROLINSKA INSTITUTET
THE NOBEL ASSEMBLY AT THE KAROLINSKA INSTITUTE
The Nobel Assembly at the Karolinska Institute has today decided to award the Nobel Prize in Physiology or Medicine for 1990 jointly to
Joseph E. Murray and E. Donnall Thomas
for their discoveries concerning “organ and cell transplantation in the treatment of human disease”.
Summary
This year’s Nobel Prize in Physiology or Medicine is given for discoveries that have enabled the development of organ and cell transplantation into a method for the treatment of human disease.
Joseph E. Murray discovered how rejection following organ transplantation in man could be mastered, and E. Donnall Thomas managed to diminish the severe reaction that the graft can cause in the recipient, i.e. the so-called “graft-versus-host” reaction (GVH). In addition, Thomas could show that intraveneously infused bone marrow cells were able to repopulate the bone marrow and produce new blood cells.
Murray successfully transplanted a kidney between homozygous twins for the first time. He pioneered transplantation of kidneys obtained from deceased persons and could show that patients with terminal renal insufficiency could be cured. The field was then open for transplantation of other organs such as liver, pancreas and heart.
Thomas was successful in transplanting bone marrow cells from one individual to another. Bone marrow transplantation can cure severe inherited disorders such as thalassemia and disorders of the immune system as well as leukemia and aplastic anemia.
Murray’s and Thomas’ discoveries are crucial for those tens of thousands of severely ill patients who either can be cured or be given a decent life when other treatment methods are without success.
Background to Organ and Cell Transplantation
The idea to transplant organs from one human being to another was raised already during ancient times. Unsuccessful attempts to transplant organs were made already around the turn of this century. The Nobel Prize Laureate in Physiology or Medicine in 1912, Alexis Carrel, concluded that there was a “biological force” that prevented successful transplantation of organs between individuals. As late as at the end of the 1940s, the Nobel Laureate in Physiology or Medicine, Sir Peter Medawar, claimed that this biological force “forever will inhibit transplantation from one individual to another”.
Many researchers did not accept this point of view. Instead, they tried to understand and define Carrel’s “biological force”, and during the 1950s and 1960s this resulted in the discoveries of specific substances on the cell surface, i.e. the so-called transplantation antigens, which in man were called HLA antigens (Human Leukocyte Antigens). The HLA antigens on the cell surface of transplanted organs are recognized by the recipient’s immune defence as foreign and immunologically active cells try to reject the graft. Following transplantation of immunologically active cells – as in bone marrow transplantation – also the cells of the recipient are recognized as foreign, and the graft reacts against the cells of the recipient in a way that can cause death. This reaction is called the “graft-versus-host” reaction (GVH) and causes “graft-versus-host disease” (GVHD). It now became a main task to develop means to master these reactions in order to make it possible to transplant both organs and cells.
This year’s Laureates paved the way for transplantation in man. The discovery that ionizing irradiation and cytotoxic drugs inhibit cell proliferation made it possible to suppress the activity of the immune cells during transplantation. Joseph E. Murray was leading in showing that total body irradiation diminished the risk of rejection of the transplanted organ. Later he could show that a still better effect was obtained with the cytotoxic drug azathioprine. E. Donnall Thomas on the other hand managed to diminish the “graft-versus-host” reaction by using another cytotoxic drug, methotrexate. Thereby the way was opened for transplantation of the bone marrow cells.
Transplantation as a Treatment Method
Organ transplantation is a surgical treatment method. An organ that has been removed from living or deceased donors has to be taken care of rapidly. Immunologically active cells still present in the vessels of the organ must be washed away. The organ has then to be surgically inserted into the recipient and induced to function. In addition, the immunological rejection reaction must be prevented.
Murray was the first to successfully transplant one kidney from one homozygous twin to the other. Thereafter, he showed that this could be done also between individuals that are not genetically identical. The prerequisite was an optimal immunosuppression. The rejection prevention has thereafter successively improved. Tens of thousands of kidney transplantations are performed in the world each year (Figure 1), and the graft survival has gradually improved and is today about 80 percent of transplanted kidneys (Figure 2).
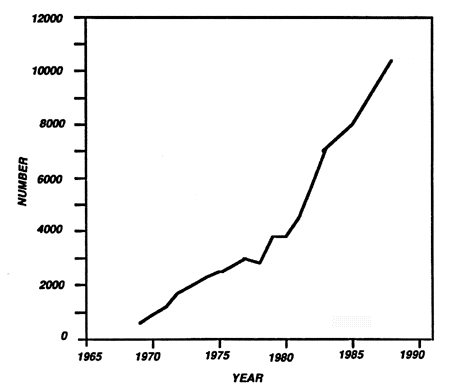 |
Figure 1. Number of kidney transplants from 1965 to 1990. Data obtained from the registry of the European Dialysis and Transplant Association/European Renal Association.
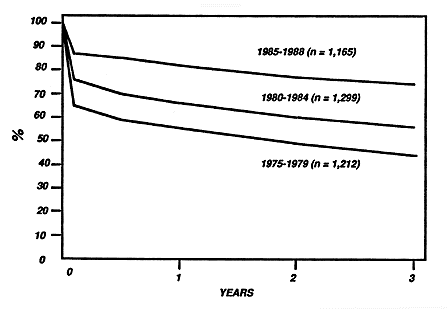
Figure 2. Results of transplantation with cadaver kidneys. Percentage survival one to three years after transplantation (from A.P.S. Disney: Clinical Transplants 1989, P. Terasaki, Ed. UCLA Tissue Typing Laboratory, Los Angeles, California).
The technique for bone marrow cell transplantation does not require surgical intervention. The marrow cells are aspirated, most often from the iliac crest of the donor. Following the killing by total body irradiation or cytotoxic drugs of the recipient’s own bone marrow and immunological defence cells the aspirated bone marrow cells are infused as in a blood transfusion. Stem cells repopulate the marrow of the recipient and give rise to both blood and immunologically active cells. Immunosuppressive treatment is given for some months to prevent or diminish the GVH reaction. The immunologically active donor cells eventually become tolerant after which the treatment can usually be withdrawn.
Since bone marrow cell transplantation means that new stem cells continually give rise to normal blood cells it is possible to cure severe blood disorders caused by inherited factors. This is true for severe blood disorders such as thalassemia and also for other inherited disorders caused by deficiences in bone marrow or immunologically active cells like severe combined immunodeficiency disease. However, the most important indications for bone marrow transplantation today are different types of leukemia (Figure 3). In chronic myeloid leukemia bone marrow transplantation is the only method which can cure the patient.
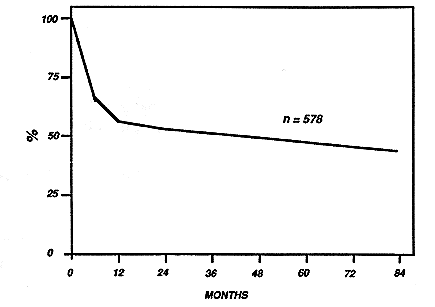 |
Figure 3. Disease-free survival following bone marrow transplantation (HLA-identical sibling donors) because of acute myeloid leukemia in first complete remission. Data from the European Group for Bone Marrow Transplantation 1988.
Every year several thousands of bone marrow transplantations are carried out in the world (Figure 4). Lately autologous bone marrow cell transplantation has been introduced. Extremely high doses of ionizing irradiation or cytotoxic drugs must sometimes be used for the treatment of certain cancers. However, this may cause a lethal damage to the patient’s bone marrow. In autologous bone marrow cell transplantation bone marrow cells from the patient are obtained before the start of the intensive treatment. After the treatment the patient is saved by reinfusion of his own bone marrow cells.
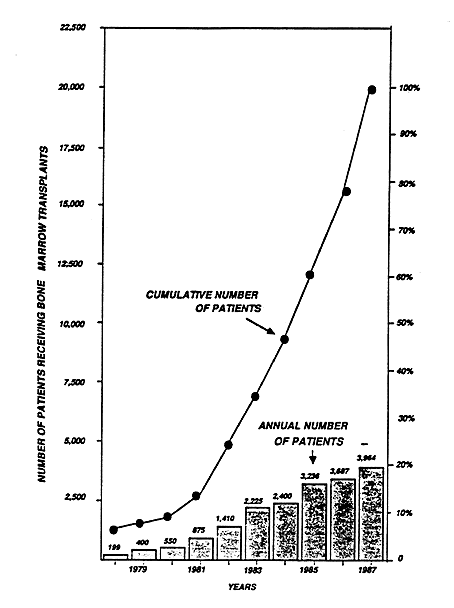
Figure 4. Number of allogeneic bone marrow transplantations (allogeneic=marrow from a donor that is not the patient himself). Worldwide data obtained from an inquiry carried out by the International Bone Marrow Transplant Registry 1987.
Literature
Groth, C-G.: Njurtransplantation i Sverige 25 år. Medicinsk kommentar. Läkartidningen 1989, 86, 4589-91.
Morris, P.J. (ed). Kidney Transplantation. Principles and Practice. W.B. Saunders Company, 1988.
Gale, R.P. & Champlin, R.E. (eds) Bone Marrow Transplantation. Current Controversies. Alan R. Liss, Inc., New York, 1989.
Gahrton, G. & Lundh, B. (eds). Blodsjukdomar. Lärobok i hematologi. Bokförlaget Natur och Kultur, Stockholm, 1983.
Gahrton, G., Ringdén, O. & Robèrt, K-H. Benmärgstransplantation – snabb utveckling mot nya indikationer. Läkartidningen 1988, 85, 689-695.
Nobel Prizes and laureates
Six prizes were awarded for achievements that have conferred the greatest benefit to humankind. The 14 laureates' work and discoveries range from quantum tunnelling to promoting democratic rights.
See them all presented here.
