Press release
English
Swedish

3 October 2005
The Nobel Assembly at Karolinska Institutet has today decided to award
The Nobel Prize in Physiology or Medicine for 2005 jointly to
Barry J. Marshall and J. Robin Warren
for their discovery of “the bacterium Helicobacter pylori and its role in gastritis and peptic ulcer disease“
Summary
This year’s Nobel Laureates in Physiology or Medicine made the remarkable and unexpected discovery that inflammation in the stomach (gastritis) as well as ulceration of the stomach or duodenum (peptic ulcer disease) is the result of an infection of the stomach caused by the bacterium Helicobacter pylori.
Robin Warren (born 1937), a pathologist from Perth, Australia, observed small curved bacteria colonizing the lower part of the stomach (antrum) in about 50% of patients from which biopsies had been taken. He made the crucial observation that signs of inflammation were always present in the gastric mucosa close to where the bacteria were seen.
Barry Marshall (born 1951), a young clinical fellow, became interested in Warren’s findings and together they initiated a study of biopsies from 100 patients. After several attempts, Marshall succeeded in cultivating a hitherto unknown bacterial species (later denoted Helicobacter pylori) from several of these biopsies. Together they found that the organism was present in almost all patients with gastric inflammation, duodenal ulcer or gastric ulcer. Based on these results, they proposed that Helicobacter pylori is involved in the aetiology of these diseases.
Even though peptic ulcers could be healed by inhibiting gastric acid production, they frequently relapsed, since bacteria and chronic inflammation of the stomach remained. In treatment studies, Marshall and Warren as well as others showed that patients could be cured from their peptic ulcer disease only when the bacteria were eradicated from the stomach. Thanks to the pioneering discovery by Marshall and Warren, peptic ulcer disease is no longer a chronic, frequently disabling condition, but a disease that can be cured by a short regimen of antibiotics and acid secretion inhibitors.
Peptic ulcer – an infectious disease!
This year’s Nobel Prize in Physiology or Medicine goes to Barry Marshall and Robin Warren, who with tenacity and a prepared mind challenged prevailing dogmas. By using technologies generally available (fibre endoscopy, silver staining of histological sections and culture techniques for microaerophilic bacteria), they made an irrefutable case that the bacterium Helicobacter pylori is causing disease. By culturing the bacteria they made them amenable to scientific study.
In 1982, when this bacterium was discovered by Marshall and Warren, stress and lifestyle were considered the major causes of peptic ulcer disease. It is now firmly established that Helicobacter pylori causes more than 90% of duodenal ulcers and up to 80% of gastric ulcers. The link between Helicobacter pylori infection and subsequent gastritis and peptic ulcer disease has been established through studies of human volunteers, antibiotic treatment studies and epidemiological studies.
Helicobacter pylori causes life-long infection
Helicobacter pylori is a spiral-shaped Gram-negative bacterium that colonizes the stomach in about 50% of all humans. In countries with high socio-economic standards infection is considerably less common than in developing countries where virtually everyone may be infected.
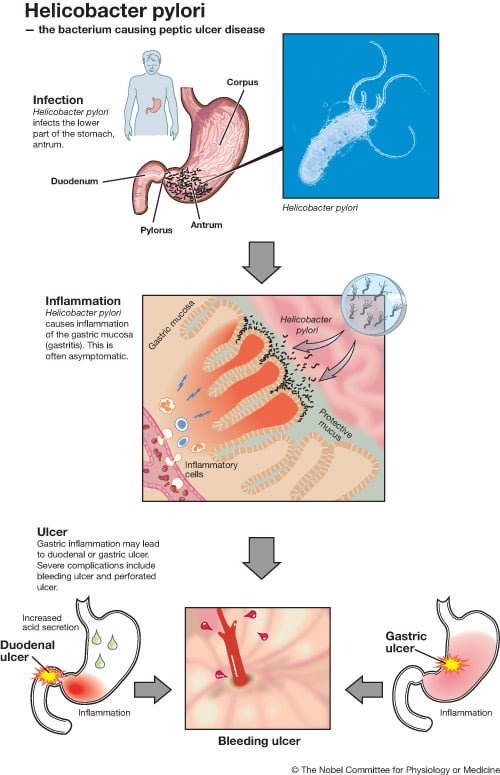
Infection is typically contracted in early childhood, frequently by transmission from mother to child, and the bacteria may remain in the stomach for the rest of the person’s life. This chronic infection is initiated in the lower part of the stomach (antrum). As first reported by Robin Warren, the presence of Helicobacter pylori is always associated with an inflammation of the underlying gastric mucosa as evidenced by an infiltration of inflammatory cells.
The infection is usually asymptomatic but can cause peptic ulcer
The severity of this inflammation and its location in the stomach is of crucial importance for the diseases that can result from Helicobacter pylori infection. In most individuals Helicobacter pylori infection is asymptomatic. However, about 10-15% of infected individuals will some time experience peptic ulcer disease. Such ulcers are more common in the duodenum than in the stomach itself. Severe complications include bleeding and perforation.
The current view is that the chronic inflammation in the distal part of the stomach caused by Helicobacter pylori infection results in an increased acid production from the non-infected upper corpus region of the stomach. This will predispose for ulcer development in the more vulnerable duodenum.
Malignancies associated with Helicobacter pylori infection
In some individuals Helicobacter pylori also infects the corpus region of the stomach. This results in a more widespread inflammation that predisposes not only to ulcer in the corpus region, but also to stomach cancer. This cancer has decreased in incidence in many countries during the last half-century but still ranks as number two in the world in terms of cancer deaths.
Inflammation in the stomach mucosa is also a risk factor for a special type of lymphatic neoplasm in the stomach, MALT (mucosa associated lymphoid tissue) lymphoma. Since such lymphomas may regress when Helicobacter pylori is eradicated by antibiotics, the bacterium plays an important role in perpetuating this tumour.
Disease or not – interaction between the bacterium and the human host
Helicobacter pylori is present only in humans and has adapted to the stomach environment. Only a minority of infected individuals develop stomach disease. After Marshall’s and Warren’s discovery, research has been intense. Details underlying the exact pathogenetic mechanisms are continuously being unravelled.
The bacterium itself is extremely variable, and strains differ markedly in many aspects, such as adherence to the gastric mucosa and ability to provoke inflammation. Even in a single infected individual all bacteria are not identical, and during the course of chronic infection bacteria adapt to the changing conditions in the stomach with time.
Likewise, genetic variations among humans may affect their susceptibility to Helicobacter pylori. Not until recently has an animal model been established, the Mongolian gerbil. In this animal, studies of peptic ulcer disease and malignant transformation promise to give more detailed information on disease mechanisms.
Antibiotics cure but can lead to resistance
Helicobacter pylori infection can be diagnosed by antibody tests, by identifying the organism in biopsies taken during endoscopy, or by the non-invasive breath test that identifies bacterial production of an enzyme in the stomach.
An indiscriminate use of antibiotics to eradicate Helicobacter pylori also from healthy carriers would lead to severe problems with bacterial resistance against these important drugs. Therefore, treatment against Helicobacter pylori should be used restrictively in patients without documented gastric or duodenal ulcer disease.
Microbial origin of other chronic inflammatory conditions?
Many diseases in humans such as Crohn’s disease, ulcerative colitis, rheumatoid arthritis and atherosclerosis are due to chronic inflammation. The discovery that one of the most common diseases of mankind, peptic ulcer disease, has a microbial cause, has stimulated the search for microbes as possible causes of other chronic inflammatory conditions.
Even though no definite answers are at hand, recent data clearly suggest that a dysfunction in the recognition of microbial products by the human immune system can result in disease development. The discovery of Helicobacter pylori has led to an increased understanding of the connection between chronic infection, inflammation and cancer.
Nobel Prizes and laureates
Six prizes were awarded for achievements that have conferred the greatest benefit to humankind. The 14 laureates' work and discoveries range from quantum tunnelling to promoting democratic rights.
See them all presented here.
